ABDOMINAL CONTOURING OPTIONS: WHAT IS THE DIFFERENCE BETWEEN A TUMMY TUCK AND A PANNICULECTOMY?
Maybe you are a hard-working mom of two who wants to get rid of the fold of skin in your lower abdomen, or you are a middle-aged man that had large weight loss after bariatric surgery with redundant skin folds, or you’re a young person who has worked hard on your diet but have extra lower abdomen tissue that gets in the way when exercising. Abdominal contouring surgery is commonly pursued following childbirth, significant weight loss, or when diet and fitness efforts fail to eliminate loose tissues of the belly. Excess fat that overhangs one’s pants, causes back pain, or prevents participation in activities is a nuisance that you don’t have to live with. But what is the procedure called to remove it? Well, there may be multiple options, but essentially there are likely two major different types of excisional (or tissue removal) ways to treat extra lower abdominal tissue: tummy tuck (or abdominoplasty) and panniculectomy. This describes the general concepts about which you may need.
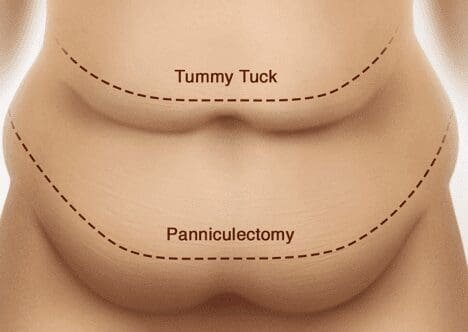
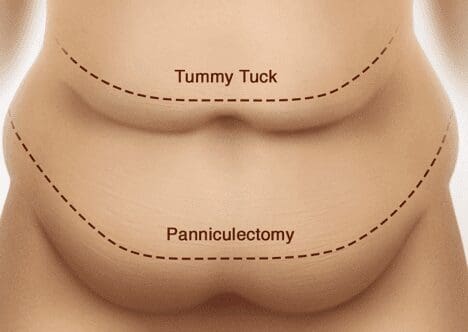
An abdominoplasty, or tummy tuck, not only removes the extra skin and soft tissue of the lower abdomen but can also further shape the upper abdomen and lateral flanks with liposuction, as well as tighten the deep abdominal wall with what is called a “rectus plication.” So, while an abdominoplasty removes extra tissue in the vertical direction, this combination of procedures also improves the horizontal contour as well. A tummy tuck is fundamentally an aesthetic procedure that is meant to improve the appearance of the entire abdomen. It is virtually never covered by insurance and is typically performed in an ambulatory surgical center.
Unfortunately, sometimes an abdominoplasty is not an option for some patients. This is to mitigate risk of complications after an abdominoplasty, which is a larger surgery with greater risk for less-than-ideal surgical candidates. The most common limiting factor is usually body-mass index (BMI), which is a ratio of a patient’s weight to their height, which if over 35 (or ideally 30), prevents performing a tummy tuck. Medical issues that are less well-controlled, advanced age, abdominal scarring or other suboptimal soft tissue issues may be other reasons that prohibit an abdominoplasty.
A panniculectomy can be thought of as a “half-abdominoplasty.” This is a procedure that only treats the lower half of the abdominal tissue by removal of the excess skin and soft tissue of the lower abdominal fold. This can help with the elimination of skin-to-skin contact regions (or “intertriginous tissue”) so that rashes, ulceration areas, fungal infections, and other skin issues may be eliminated. Panniculectomy is designed to help with the contour of the lower abdomen and does not improve the shape of the upper abdomen or tissue around the belly button. The lower abdominal tissue only is removed in a panniculectomy, and the belly button, or umbilicus, is left in its native location. No rectus muscle plication, or deep “fascia” level tightening is conducted in this procedure, nor is there any upper abdominal contouring involved. Panniculectomy also does not treat the deep layers, such as the strong tissue called fascia that lies over the abdominal muscles and can cause a “rectus diastasis,” or pseudo-hernia, of the abdominal wall, which are typically repaired during an abdominoplasty. Liposuction is also not used typically during a panniculectomy, so there is little lateral abdominal contouring during a panniculectomy. It is simply the removal of the fold of excess skin and fat of the lower abdomen. While there is less cosmetic benefit from panniculectomy, it is the safer procedure for some patients and panniculectomy does not prevent a future abdominoplasty.
If you are interested in an abdominal contouring procedure but do not know which you are a candidate for, then feel free to reach out for a consultation. Dr. Day has extensive experience in abdominoplasty, panniculectomy, and a range of other abdominal contouring techniques and will design a customized approach to help you achieve your best results!